Breast cancer is the commonest cancer in Nigeria. It accounts for 38% of all cancer cases in Nigeria. About 40 women die daily from breast cancer in the country making it the highest cancer killer in Nigeria - higher than cervical and prostate cancer fatalities combined. Early diagnosis of breast cancer coupled with accurate and timely treatment lead to better outcomes.
According to the World Health Organisation, a third of cancers can be prevented. With early detection another third can be cured. With a few lifestyle changes, we can lower the risk of developing some cancers. Here are some of these changes:

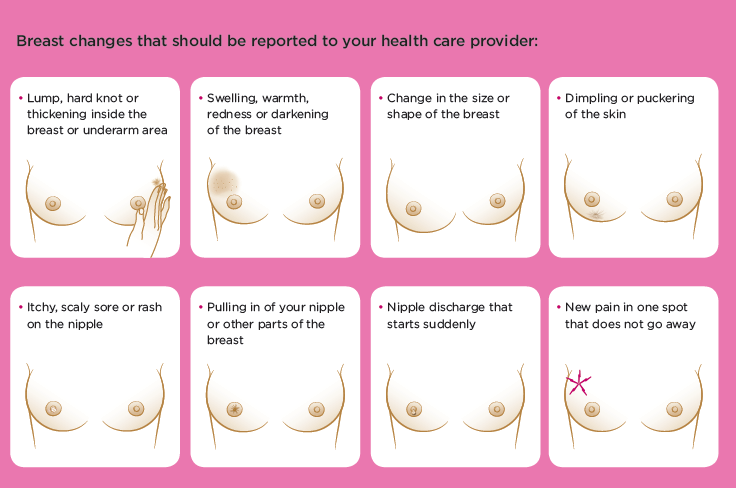
Although a lump is the most common sign of breast cancer, there are actually other warning signs you need to know about. Also, some of these warning signs are visual changes that cannot be felt.⠀⠀
In most cases, these changes may not be cancer, however if you experience any of the above, see your healthcare provider immediately.
Also, if you’ve had a benign lump in the past, don’t assume a new lump will also be benign. The new lump may not be breast cancer, but it’s best to make sure.
Ladies, ensure you do your regular breast checks. Remember, early detection and treatment saves lives.
Source: CancerAware.
Some of the factors below increase the risks of cancer:.

What does a lump feel like?
Breast cancer lumps don’t all feel the same. Your doctor should examine any lump, whether or not it meets the most common symptoms listed below.⠀⠀
Most commonly, a cancerous lump in the breast:
- is a hard mass
- is painless
- has irregular edges
- is immobile (doesn’t move when pushed)
- appears in the upper outer portion of your breast
- grows over time
Not all cancerous lumps will meet these criteria, and a cancerous lump that has all of these traits isn’t typical. A cancerous lump may feel rounded, soft, and tender and can occur anywhere in the breast. In some cases, the lump can even be painful.
Some women also have dense, fibrous breast tissue. Feeling lumps or changes in your breasts may be more difficult if this is the case.
Having dense breasts also makes it more difficult to detect breast cancer on mammograms. Despite the tougher tissue, you might still be able to identify when a change begins in your breast.
Breast cancer in men
Most breast cancers are diagnosed in women. However, men do have breast tissue and can develop breast cancer. Still, less than one percent of all breast cancers occur in men.
Symptoms of breast cancer in men are the same as the symptoms of breast cancer in women. These symptoms include:
- a lump in one breast
- a nipple that turns inward (inverts)
- nipple pain
- discharge from the nipple
- redness, dimpling, or scaling on the breast’s skin
- redness or sores on the nipple or ring around the nipple
- swollen lymph nodes in armpits
As with women, breast cancer in men can spread or metastasize to other parts of the body. Diagnosing the cancer in early stages important. This way, you and your doctor can quickly begin treating the cancer.
While breast cancer is rare in men, some common risk factors are known.
What is male breast cancer?
Breast cancer happens when cells grow out of control inside the breast. Cancer in the breast can spread to other parts of the body.
Breast cancer isn’t only a woman’s disease. Men can also get breast cancer, although it’s rare.
Symptoms of male breast cancer are the same as those in women. But because men don’t regularly check their breasts or get mammograms, the signs are easier to miss.
It’s important to note that breast enlargement in men isn’t a sign of breast cancer. When this happens, it’s called gynecomastia, and it may be due to weight gain or the use of certain medicines.
But men don’t have breasts, do they?
Men do have breast tissue, just like women. The difference is in the amount of tissue they have.
Before puberty, boys and girls have the same amount of breast tissue. Breast tissue is made up of milk-producing glands called lobules, ducts that transport milk to the nipples, and fat.
At puberty, girls’ ovaries start producing female hormones. These hormones cause the breasts to grow. Boys don’t produce the same hormones, so their breasts stay flat. Sometimes a man’s breasts can grow because he takes certain hormones or if he’s exposed to hormones in the environment..
Men can develop a few different types of breast cancer:
- Ductal carcinoma is an early cancer that starts in the milk ducts.
- Lobular carcinoma starts in the milk-producing glands.
- Paget disease starts in the breast ducts, and then spreads to the nipple.
- Inflammatory breast cancer makes the breast swell up and turn red. It’s very rare, but also very ag-gressive.
Who’s at risk?
Although breast cancer is rare in men, it’s important to know if you’re at risk. That’s because men aren’t routinely screened for breast cancer like women are.
Risks for male breast cancer include:
Age: Whether you’re a man or a woman, you’re more likely to get breast cancer as you get older. The average age for a man to get diagnosed is 68. However, you can get breast cancer at any age.
Genes: Breast cancer runs in families. If your father, brother, or other close relatives were diagnosed, you may also be at risk. Certain genes increase your likelihood of getting this cancer — including the BRCA1 and BRCA2 genes. These genes code for proteins that prevent breast cells from growing out of control. Both men and women who inherit the BRCA1 or BRCA2 gene mutations are at increased risk for breast cancer, although their risk is still small. Your lifetime risk of breast cancer is about 1 percent if you have the BRCA1 gene, and 6 percent if you have the BRCA2 gene.
Weight gain: Fat tissue releases the female hormone estrogen. Estrogen stimulates breast cancer growth. The more overweight you are, the more of this hormone you produce.
Hormone exposure: You’re at higher risk for breast cancer if you take hormone-based drugs (for example, to treat prostate cancer), or if you were exposed to estrogen through food, pesticide, or other products.
Klinefelter syndrome: This condition causes men to be born with an extra copy of the X chromosome. Normally, men have one X and one Y chromosome (XY). In Klinefelter syndrome, they have two copies of the X chromosome in addition to the Y chromosome (XXY). Men with this condition have smaller than normal testicles. They make less testosterone and more estrogen than usual. Men with Klinefelter syndrome are at greater risk for breast cancer.
Heavy alcohol use: Drinking a lot of alcohol can cause estrogen levels in your blood to rise.
Liver disease: Cirrhosis and other diseases that damage the liver can reduce the amount of male hormones and increase the amount of estrogen in your body.
Surgery to your testicles: Damage to your testicles can increase your risk for breast cancer..
Radiation exposure: Radiation is linked to breast cancer. If you received radiation to the chest to treat another type of cancer, you could be at greater risk for breast cancer..
How common is male breast cancer?
Breast cancer in men is rare, but it can still happen. Men make up less than 1 percent of all breast cancer cases. A man’s risk of getting breast cancer during his lifetime is about 1 in 1,000.
The disease is much less common in men because their breast ducts — where the cancer starts — are less well-developed than women’s. Men also have lower levels of estrogen, the hormone that fuels breast cancer growth.
Is it serious?
Breast cancer can spread to other parts of the body, which makes it more serious. Male breast cancer is just as serious as female breast cancer.
Your outlook depends on what type of cancer you have and how quickly you’re diagnosed. Your odds of being cured are highest if you catch the cancer early. The five-year relative survival rate for a man with stage 0 or stage 1 breast cancer is 100 percent. That’s why it’s important to check your breasts regularly, and alert your doctor right away if you spot any symptoms of breast cancer.
How to reduce your risk?
Many risks for breast cancer — like family history and age — are out of your control. But there are a few risk factors you can control, including obesity.
Here are some tips to help lower your odds of getting breast cancer:
- Keep your weight within a healthy range. Obesity can shift the hormone balance in your body, making you more likely to get breast cancer. If you’re overweight, talk to your doc-tor and a dietician about making changes to your eating and exercise plan.
- Exercise on most days of the week. A lack of physical activity can alter your hormone levels, making you more susceptible to cancer.
- Avoid or limit alcohol. Having two or more alcohol drinks daily has been linked to an in-creased risk for breast cancer in women. Even though the link isn’t as clear in men, it’s still worth cutting back.
If male breast cancer runs in your family, you may not be able to prevent it. However, you can catch it early by knowing your risk. Talk to a genetic counsellor about getting tested for BRCA1, BRCA2, and other genes.
How to perform a self-exam
Screening techniques help you and your doctor identify suspicious spots in your breast. A mammogram is a common screening option. A breast self-exam is another.
The self-exam was considered an important part of early breast cancer detection for many decades. Today, however, it may lead to too many unnecessary biopsies and surgical procedures.
Still, your doctor may recommend a self-exam to you. At the very least, the exam can help you familiarize yourself with your breasts’ appearance, shape, texture, and size. Knowing what your breasts should feel like could help you spot a potential problem more easily.
How to Check Yourself
Source: Susan G Komen
- Pick a date. Hormones impact how your breasts feel, so it’s a good idea to wait a few days after your menstrual cycle ends. If you do not have a period, pick a date on the calendar you can easily remember, such as the first or fifteenth, and schedule your self-exam.
- Take a look. Remove your top and bra. Stand in front of a mirror. Observe how your breasts look, inspecting them for changes in symmetry, shape, size, or colour. Raise both arms, and repeat the visual inspection, noting the changes to your breasts’ shape and size when your arms are extended.
- Inspect each breast. Once you’ve completed the visual exam, lie down on a bed or sofa. Use the soft pads of your fingers to feel for lumps, cysts, or other abnormalities. To keep the inspection uniform, start at your nipple and work your way out, to your breastbone and armpit, in a spiral pattern. Repeat on the other side.
- Squeeze your nipple. Gently squeeze on each nipple to see if you have any discharge.
- Repeat in the shower. Do one final inspection in the shower. Let warm water and soap make the manual examination easier by gliding your fingers over your breasts. Start at your nipple and work your way out in a spiral pattern. Repeat on the other breast.
- Keep a journal Subtle changes may be hard to detect, but a journal might help you see developments as they occur. Jot down any unusual spots and check them again in a few weeks. If you find any lumps, see your doctor.
Other conditions that can cause breast lumps
Breast cancer is not the only condition that can cause unusual lumps in your breasts. These other conditions might also be responsible:
- swollen lymph nodes
- cysts
- bacterial of viral infection
- a skin reaction to shaving or waxing
- allergic reactions
- a noncancerous tissue growth (fibro adenoma)
- a fatty tissue growth (lipoma)
- lymphoma
- leukaemia
- lupus
- swollen or clogged mammary glands
A lump in your armpit or breasts is unlikely to be breast cancer, but you should talk with your doctor about any unusual spots to find. Your doctor will likely perform a physical exam and rule out possible causes for unusual lumps.
The takeaway
Your body is your own, and it’s the only one you have. If you find a lump or you’re experiencing any unusual symptoms, you should seek out your doctor’s guidance.
Your doctor may be able to determine from a physical exam whether your lump is likely to be cancerous. If you’re at all concerned about the new signs and symptoms, you shouldn’t be afraid to request additional testing to diagnose your lump.